Did you know that according to the British Heart Foundation, approximately 14.4 million adults in the UK live with high blood pressure, but nearly 5 million of those cases are currently undiagnosed? It's a statistic that highlights why regular monitoring and understanding a blood pressure chart are fundamental pillars of modern health preservation. You might find yourself staring at a digital screen, feeling a flicker of anxiety as you try to decipher what those two numbers actually mean for your heart. It's common to feel confused about the relationship between systolic and diastolic pressures or to wonder if your home device is providing the clinical accuracy you require.
We understand that true peace of mind comes from clarity and professional insight rather than guesswork. This guide provides a definitive breakdown of cardiovascular categories updated for 2026, designed to help you master your health data with absolute confidence. You'll learn to interpret your specific risk levels, discover the most effective ways to support your vascular health naturally, and understand exactly when it's time to consult your GP. From perfecting your home measurement technique to exploring high-potency lifestyle interventions, we're here to ensure your journey toward heart health is both informed and sustainable.
Key Takeaways
- Understand why hypertension is considered a "silent killer" and how proactive monitoring serves as a vital tool for early cardiovascular intervention.
- Learn to decode the difference between systolic and diastolic pressures to interpret the clinical significance of your mmHg readings.
- Utilise our detailed blood pressure chart to categorise your results and identify whether you are within the ideal range or the pre-hypertension "warning zone".
- Master the "Rule of Two" for home monitoring to ensure your data is accurate and ready for clinical review by your healthcare provider.
- Discover how managing your weight through modern pharmaceutical support can directly improve your arterial health and overall cardiovascular wellbeing.
What is a Blood Pressure Chart and Why Does It Matter?
A blood pressure chart is much more than a simple reference grid; it's a vital clinical tool used to categorise heart health based on the force your blood exerts against arterial walls. By plotting your systolic and diastolic readings, you can immediately identify if your cardiovascular system is under unnecessary strain. This visual data is essential for a deeper understanding of hypertension, a condition that affects roughly 14 million adults in the UK. Without this tool, many individuals remain unaware of their risk levels because high blood pressure rarely presents obvious physical warning signs.
Monitoring these figures is a primary defence against what clinicians call the "silent killer." Hypertension often progresses for years without causing headaches or dizziness. By the time symptoms appear, the damage to the arteries might already be extensive. Consistent use of a chart helps in the early detection and prevention of life-altering events such as strokes, myocardial infarctions, and chronic kidney failure. At SW Pharma, we focus on providing regulated UK pharmacy services that empower patients to take control of these metrics before they escalate into emergencies.
The Importance of Proactive Cardiovascular Monitoring
Adopting a reactive approach to heart health is a dangerous strategy. Waiting for your body to "tell" you something is wrong often leads to late-stage diagnoses. Projections for 2026 indicate that over 8.1 million people in the UK will be living with a heart or circulatory disease, a figure driven by an ageing population and rising metabolic health challenges. Early intervention is the only way to shift these statistics. Hypertension is a leading cause of avoidable death in the UK. Regular tracking allows for lifestyle adjustments or pharmacological interventions that can reduce stroke risk by up to 40% and heart failure risk by 50%.
Who Should Regularly Check the Chart?
While everyone should know their numbers, certain groups face higher risks. NHS guidelines recommend that all adults over the age of 40 have their blood pressure checked at least every five years. However, if your Body Mass Index (BMI) is over 25, more frequent monitoring is necessary. Excess weight forces the heart to work harder, which often leads to elevated readings that a blood pressure chart can help track over time.
Those currently enrolled in weight management programmes should be particularly vigilant. As you lose weight, your blood pressure often drops, which might require adjustments to any existing medications. You can consult SW Pharma, a GPhC-registered source, for professional health advice and support in managing your cardiovascular profile. Tracking your progress on a chart provides the data your pharmacist or GP needs to make informed decisions about your care. It's a small habit that yields significant long-term protection for your heart and kidneys.
Decoding the Numbers: Systolic vs Diastolic Pressure
Understanding your blood pressure reading starts with the unit mmHg, which stands for millimetres of mercury. Even though modern digital monitors don't use liquid mercury, this remains the global clinical standard for measuring pressure. Your reading consists of two distinct figures, usually written as one over the other. The top number represents systolic pressure, while the bottom reflects diastolic pressure. Both figures provide a window into different aspects of your cardiovascular health, and a single high reading in either category can be a cause for clinical review.
The British Heart Foundation reports that approximately 14.4 million people in the UK live with high blood pressure, yet many don't understand what these two numbers actually signify. Doctors treat both values with equal importance because they reveal how your heart and blood vessels behave during different phases of the cardiac cycle. While they work together, they respond to different physiological triggers and lifestyle factors.
What the Top Number (Systolic) Tells You
Systolic blood pressure is the maximum force your heart exerts against your artery walls each time it beats. This number is often the primary focus for healthcare professionals when assessing cardiovascular risk in patients over 50. As we age, our large arteries naturally lose some of their elasticity and become stiffer. This stiffening, often combined with long-term plaque buildup, causes the systolic pressure to rise as the heart works harder to circulate blood.
When you consult a blood pressure chart, you'll see that a high systolic reading indicates immediate stress on your system. If this top number is consistently 140 mmHg or higher, it suggests your heart is under significant strain during its most active phase. This persistent pressure can weaken the heart muscle over time and damage the delicate lining of the arteries, increasing the risk of stroke or heart attack.
What the Bottom Number (Diastolic) Tells You
The diastolic number represents the pressure in your arteries when your heart rests between beats. It's the period when the heart refills with blood and receives its own oxygen supply. While systolic pressure focuses on the "work" phase, the diastolic reading focuses on the "rest" phase. It measures the minimum amount of pressure your blood vessels must withstand at all times, reflecting the overall resistance in your peripheral vascular system.
For younger adults, specifically those under 40, a high diastolic reading is often a more significant predictor of future health complications. If your diastolic pressure remains high, it means your blood vessels never get a chance to fully relax. This constant tension is often linked to high salt intake, obesity, or a lack of physical activity. Ensuring your vessels remain flexible is vital; incorporating a high-quality supplement into a balanced lifestyle can support vascular health and help maintain natural equilibrium.
- Systolic (Top): Measures pressure during the heartbeat. It's highly sensitive to age, stress, and physical activity.
- Diastolic (Bottom): Measures pressure during the heart's resting phase. It indicates the health of smaller blood vessels.
- Clinical Diagnosis: A diagnosis of hypertension can be made if either number is consistently higher than the recommended range of 120/80 mmHg.
The 2023 British and Irish Hypertension Society guidelines emphasise that both numbers are critical for a full clinical picture. You can't ignore a high bottom number just because the top one is normal, or vice versa. In fact, isolated diastolic hypertension is a common clinical finding in younger populations, while older adults more frequently experience isolated systolic hypertension. Both conditions require professional management to prevent long-term damage to the kidneys, eyes, and brain.
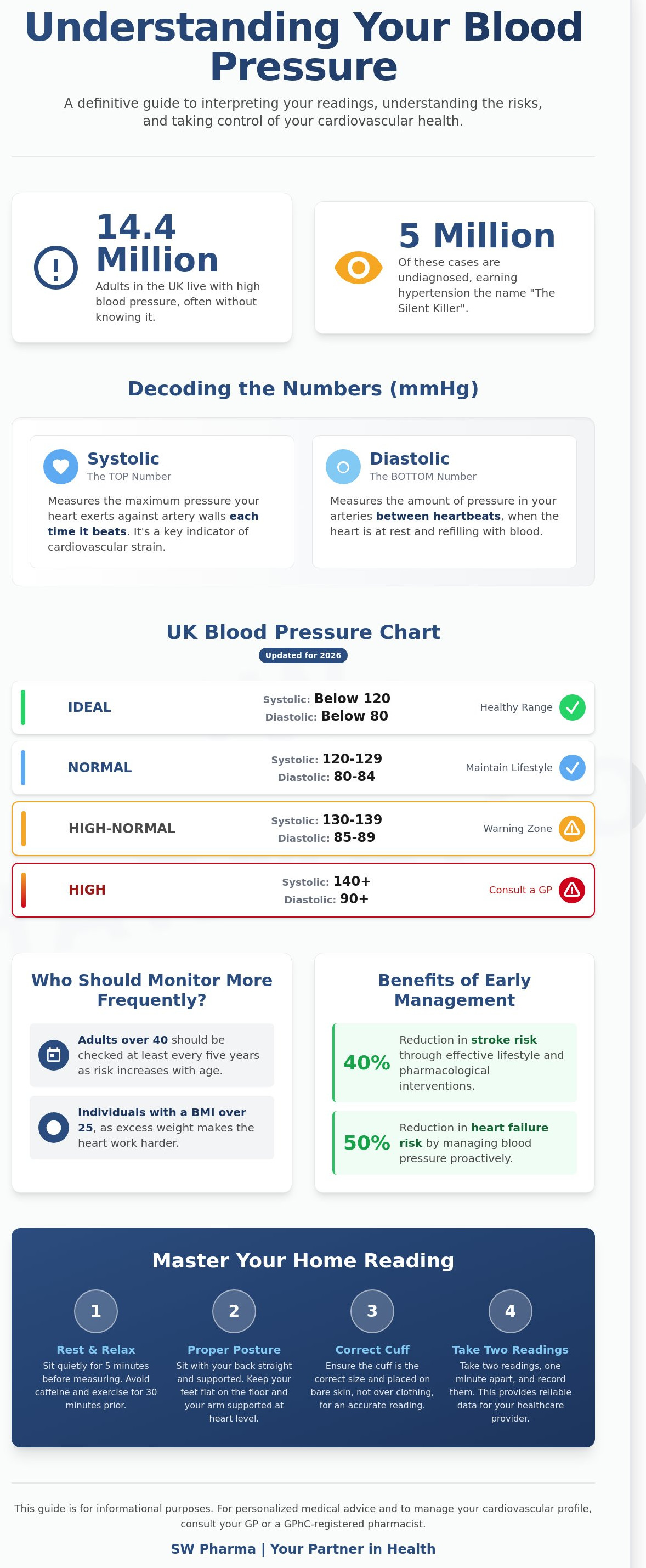
The UK Blood Pressure Chart: Categorising Your Results
A standardised blood pressure chart serves as the primary diagnostic roadmap for clinicians across the United Kingdom. It categorises readings based on the force exerted against arterial walls during and between heartbeats. Understanding these benchmarks allows for proactive health management rather than reactive treatment. The current clinical framework identifies five distinct zones that dictate the necessary level of medical or lifestyle intervention.
A reading below 120/80mmHg represents the ideal physiological state for most adults. This normal range indicates that the heart and vascular system are functioning with minimal strain, preserving the integrity of blood vessels over time. When readings climb into the 120/80mmHg to 139/89mmHg bracket, individuals enter the pre-hypertension phase. This is a critical "warning zone." Recent data suggests that approximately 5 million people in the UK are currently living with undiagnosed high blood pressure. Identifying your status in this amber zone provides a vital window for intervention through targeted lifestyle adjustments before clinical damage occurs.
Clinical hypertension is divided into two main stages. Stage 1 is diagnosed when clinic readings consistently reach 140/90mmHg. If measurements hit 160/100mmHg or higher, it's classified as Stage 2 hypertension. At these levels, the risk of cardiovascular events increases significantly, and GPs will typically discuss pharmacological options alongside habit changes. Conversely, hypotension occurs when readings drop below 90/60mmHg. While often found in highly trained athletes, low blood pressure becomes a clinical concern if it results in cognitive fog, persistent dizziness, or fainting spells.
Understanding the Colour-Coded Risk Zones
Visual blood pressure chart tools use a traffic light system to help patients track their cardiovascular health. Green signifies a healthy, low-risk state. Amber indicates elevated pressure that requires consistent monitoring. Red denotes high pressure where professional medical consultation is mandatory. It's essential to follow the latest UK blood pressure guidelines when interpreting these results to ensure accuracy.
Many patients experience the "White Coat Effect," where the anxiety of being in a GP surgery causes a temporary spike in readings. This phenomenon can inflate results by 10 to 20mmHg. Because of this, a single high reading is never used as a definitive diagnosis. Doctors prefer to see a trend over several weeks using home monitoring or a 24-hour ambulatory monitor to confirm your true baseline.
When a Reading Becomes a Medical Emergency
A hypertensive crisis is a medical emergency where blood pressure exceeds 180/120mmHg. This level of pressure can cause immediate damage to the heart, kidneys, or brain. You must seek urgent help if these high numbers are accompanied by specific red-flag symptoms. These include severe chest pain, a sudden, "thunderclap" headache, or acute changes in vision.
If you experience these symptoms alongside a high reading, you should call 999 or attend your local A&E department immediately. For situations where your reading is high but you feel otherwise well, or if you have concerns about your medication, the NHS 111 service offers 24/7 clinical advice. Prompt action in these scenarios is the most effective way to prevent long-term complications such as strokes or heart failure.
How to Take an Accurate Reading at Home: A Step-by-Step Guide
Obtaining a reliable reading requires more than just pressing a button on a digital device. Clinical accuracy depends on your physical preparation and the quality of your equipment. When you monitor your levels at home, you're looking for a stable average that reflects your true cardiovascular health, rather than a single moment influenced by stress or activity. This data helps you understand where you sit on a standard blood pressure chart and allows for more informed discussions with your healthcare provider.
Selecting a monitor isn't a task to take lightly. You should always look for a device validated by the British and Irish Hypertension Society (BIHS) or one carrying the CE mark. These certifications confirm the monitor has passed rigorous clinical testing for accuracy. Once you've got your device, you'll need to follow the "Rule of Two" to ensure your data is statistically significant. This involves taking two separate readings, spaced two minutes apart, twice every day. Performing this routine in the morning and evening provides a stable average that reflects your cardiovascular state without the interference of daily fluctuations.
Preparing for Your Measurement
Your body needs time to reach a state of haemodynamic stability before you begin. You must avoid caffeine, smoking, and vigorous exercise for at least 30 minutes before testing. These factors stimulate the nervous system and can cause temporary spikes that don't represent your resting state. Find a quiet environment where you won't be interrupted; even background noise can subtly raise your heart rate and affect the result.
Cuff size is perhaps the most overlooked factor in home monitoring. Before purchasing a device, measure your upper arm circumference at the midpoint between your shoulder and elbow. Using a cuff that's too small for your arm can add an extra 10mmHg to your reading, potentially leading to an incorrect classification of hypertension. Most standard cuffs fit arms 22 to 32 centimetres in circumference, but large-sized cuffs are available if your measurements exceed this range.
Common Mistakes That Alter Your Results
Small physical adjustments can lead to significant data errors. Sitting with your legs crossed or failing to support your back can increase your systolic pressure by several points because of the muscle tension required to maintain your posture. You should sit in a sturdy chair with your feet flat on the floor and your back firmly supported. Your arm should rest on a flat surface, such as a table, so the cuff sits at the same horizontal level as your heart.
- Don't talk during the measurement, as even quiet conversation can impact the results.
- Ensure the cuff is placed on bare skin rather than over thick clothing or rolled-up sleeves that might constrict blood flow.
- Keep your arm relaxed and still until the device has completely finished its cycle.
- Wait at least two minutes before taking a second reading to allow blood flow to return to normal.
Documenting these figures is essential for long-term health management. Maintaining a consistent blood pressure diary allows you to track patterns over weeks and months. When you compare these figures against a blood pressure chart, you can see the direct impact of lifestyle changes or new supplement regimens. Sharing this diary with your London pharmacist provides them with the evidence needed to offer tailored advice on your cardiovascular wellness.
Take control of your cardiovascular health by choosing high-quality support for your circulation. Discover our premium range of heart health supplements designed to complement your daily wellness routine.
Beyond the Chart: Managing Your Blood Pressure with SW Pharma
Understanding your numbers on a blood pressure chart is the first step toward long-term cardiovascular health. However, data alone doesn't change outcomes; targeted intervention does. At SW Pharma, we bridge the gap between diagnosis and effective management through clinical expertise and modern pharmaceutical solutions. High blood pressure, or hypertension, often acts as a silent precursor to more severe conditions, but it's a manageable risk factor when you have the right tools and professional guidance.
Weight Management as Hypertension Prevention
Excess body mass places a direct mechanical and metabolic strain on the heart. Clinical data from the British Heart Foundation indicates that losing just 5% to 10% of your total body weight can lead to a significant reduction in systolic blood pressure. For many patients, this modest shift is enough to move their readings from a "high" category on the blood pressure chart back into a healthier range. Reducing adipose tissue decreases the systemic inflammation and vascular resistance that force your heart to work harder than necessary.
Modern treatments have transformed how we approach this challenge. Medications like Mounjaro (Tirzepatide) and Wegovy (Semaglutide) aren't just about aesthetics; they're powerful tools for heart health. These treatments mimic natural incretin hormones to regulate appetite and improve insulin sensitivity. A 2023 study published in The New England Journal of Medicine showed that Semaglutide reduced the risk of major adverse cardiovascular events by 20% in adults with overweight or obesity. Before starting any treatment, it's vital to know your starting point. You can use the SW Pharma BMI calculator to establish your baseline and see if these clinical interventions are suitable for your health profile.
Dietary choices act as a foundation for any medication. The DASH (Dietary Approaches to Stop Hypertension) diet emphasizes whole grains, lean proteins, and vegetables while strictly limiting sodium. The NHS recommends consuming no more than 6g of salt per day, which is roughly one level teaspoon. Reducing salt intake by just 2g a day can lower systolic blood pressure by nearly 5 mmHg. Combine this with 150 minutes of moderate-intensity aerobic activity each week to strengthen the heart muscle. A stronger heart pumps blood with less effort, naturally lowering the pressure in your arteries.
Consulting Our London-Based Online Pharmacists
Managing hypertension requires a personalised approach rather than a one-size-fits-all solution. Our clinical team consists of London-based pharmacists registered with the General Pharmaceutical Council (GPhC). We provide a secure, online clinical assessment that reviews your medical history and current readings to ensure any prescribed medication is safe and appropriate for you.
Our process removes the barriers of traditional waiting rooms and provides a streamlined path to care. Once our clinicians approve your assessment, your treatment is dispensed from our UK-registered pharmacy and delivered discreetly to your home. We prioritise transparency and clinical safety above all else. If you're ready to take control of your cardiovascular health or need support with weight management, organise a consultation with us today. Our experts are here to help you move beyond the numbers and achieve lasting wellness through evidence-based care.
Take Proactive Control of Your Cardiovascular Health
Monitoring your heart health starts with a clear understanding of your data. A standard blood pressure chart helps you distinguish between your systolic and diastolic readings; the NHS identifies hypertension as readings consistently above 140/90mmHg. Taking accurate measurements at home requires at least five minutes of quiet rest to ensure your baseline remains stable. If your results sit outside the healthy range, you don't have to navigate the next steps alone. SW Pharma provides a direct bridge between clinical data and effective management. As a GPhC Registered Pharmacy, our London-based clinical experts offer tailored support and evidence-based treatments. We ensure your privacy with discreet UK-wide delivery, typically reaching your doorstep within 24 to 48 hours. Managing your vital signs is a lifelong commitment to your long-term vitality. You've already taken the first step by learning the science behind the stats. Now, it's time to turn that knowledge into a proactive health strategy with professional guidance. Start your online clinical assessment with SW Pharma today and move toward a more balanced and secure future.
Frequently Asked Questions
What is considered a "normal" blood pressure reading for my age?
An ideal blood pressure reading for most adults is between 90/60mmHg and 120/80mmHg. While figures can fluctuate as you age, the NHS defines hypertension as anything consistently over 140/90mmHg for adults under 80. If you're over 80, the target is slightly higher at 150/90mmHg. Checking a blood pressure chart helps you see where your specific numbers sit within these clinical categories.
Can I lower my blood pressure naturally without medication?
You can reduce your systolic pressure by up to 11mmHg through sustained lifestyle changes. Reducing daily salt intake to less than 6g and performing 150 minutes of moderate aerobic activity weekly are proven methods. These interventions improve arterial elasticity and support cardiovascular balance. Many patients find that losing just 1kg of body weight leads to a 1mmHg drop in blood pressure.
Why is my blood pressure always higher at the GP surgery than at home?
This phenomenon is known as the white coat effect, and it impacts approximately 30% of patients during clinical consultations. The stress of a medical environment triggers a temporary spike in your heart rate and vascular resistance. Doctors prefer using a blood pressure chart to compare your home readings with clinic data. This ensures they don't misdiagnose you based on a single, stress-induced measurement.
Is 140/90 considered high blood pressure in the UK?
A reading of 140/90mmHg is the threshold for Stage 1 hypertension when measured in a clinical setting. In the UK, the National Institute for Health and Care Excellence (NICE) uses this figure to identify patients at increased risk of cardiovascular events. If your home readings average 135/85mmHg or higher, your GP'll likely recommend a formal management plan to protect your long-term heart health.
What should I do if my blood pressure reading is suddenly very high?
If your reading exceeds 180/120mmHg, wait five minutes and test yourself again. A singular high reading isn't always an emergency, but sustained levels at this height require medical attention. Call 999 immediately if you experience chest pain, blurred vision, or a severe headache alongside these numbers. These symptoms may indicate an acute hypertensive crisis which needs urgent clinical intervention.
Does losing weight really help lower blood pressure?
Losing weight's one of the most effective non-pharmacological ways to control your readings. Research shows that for every kilogram of weight lost, your systolic blood pressure typically drops by 1mmHg. This happens because a lower body mass reduces the strain on your heart and improves the efficiency of your circulatory system. Maintaining a healthy BMI between 18.5 and 24.9 provides the best protection for your arteries.
How often should I check my blood pressure at home?
You should monitor your blood pressure twice daily for a full week when first establishing a baseline. Take two readings in the morning and two in the evening, spaced one minute apart. This 7-day period provides 28 individual data points for your doctor to review. Once your levels are stable, checking once a month's usually sufficient to ensure your cardiovascular health remains within the target range.


![Wegovy Side Effects Management: A Clinical Guide for UK Patients [2026]](https://getautoseo.com/storage/hero_images/article_665463_1776498695.jpg)
![Wegovy vs Saxenda for Weight Loss: A Clinical Comparison for UK Patients [2026]](https://getautoseo.com/storage/hero_images/article_1261167_1776484316.jpg)
